Understanding Septal Infarct: Causes, Symptoms, and Treatment
Septal infarct is a medical condition characterized by damage to the septum, the wall that separates the left and right sides of the heart. It occurs as a result of reduced blood flow to the septal region, leading to tissue death. In this blog post, we will delve into the causes, symptoms, and treatment options for septal infarct, shedding light on this cardiovascular condition that affects many individuals worldwide.
What Causes Septal Infarct?
Septal infarct typically occurs due to a blockage in one of the coronary arteries, which supply blood to the heart muscle. The most common cause is the formation of a blood clot or plaque buildup in the arteries. These clots or plaques obstruct the blood flow, leading to ischemia (lack of oxygen) and subsequent tissue damage. Other factors that can contribute to septal infarct include high blood pressure, smoking, diabetes, and a family history of cardiovascular disease.
Recognizing the Symptoms:
Identifying the symptoms of septal infarct is crucial for prompt diagnosis and treatment. The manifestations of this condition may vary from person to person, but common symptoms include chest pain or discomfort, shortness of breath, fatigue, dizziness, and irregular heartbeats. Some individuals may experience nausea or sweating as well. It is essential to seek immediate medical attention if you or someone you know exhibits these symptoms, as early intervention can significantly improve outcomes.
Diagnosis and Medical Evaluation:
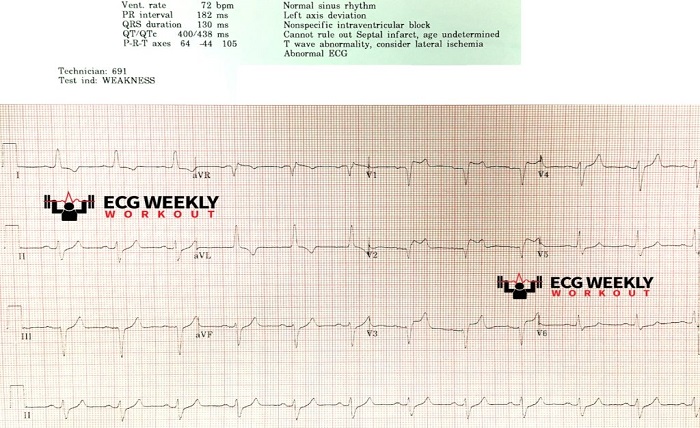
When a patient presents with suspected septal infarct, healthcare professionals conduct a thorough medical evaluation to confirm the diagnosis. This evaluation typically involves a detailed medical history review, physical examination, and several diagnostic tests. Electrocardiography (ECG) is commonly used to detect abnormalities in the heart’s electrical activity, and it can often indicate the presence of a septal infarct. Additional tests such as echocardiography, stress tests, or cardiac catheterization may be performed to assess the extent of the damage and identify any underlying conditions.
Treatment Options:
The treatment approach for septal infarct aims to alleviate symptoms, prevent further damage, and improve overall cardiac function. The specific treatment plan depends on the severity of the condition and the individual patient’s needs. In many cases, medications such as antiplatelet agents, beta-blockers, and ACE inhibitors are prescribed to reduce clot formation, control blood pressure, and improve heart function. Lifestyle modifications, including a heart-healthy diet, regular exercise, and smoking cessation, are also recommended. In severe cases, interventional procedures like angioplasty or coronary artery bypass grafting (CABG) may be necessary to restore blood flow to the heart.
Post-Infarct Care and Rehabilitation:
After surviving a septal infarct, patients require ongoing care and rehabilitation to aid their recovery process and prevent future cardiac events. Cardiac rehabilitation programs often include supervised exercise sessions, dietary guidance, medication management, and counseling to address emotional well-being. These programs play a vital role in improving the patient’s quality of life, reducing the risk of subsequent heart problems, and providing a supportive environment for their overall well-being.
Conclusion:
Septal infarct is a serious cardiovascular condition that requires timely diagnosis and appropriate treatment to prevent complications. Recognizing the symptoms and seeking medical attention promptly can make a significant difference in the outcome for individuals affected by this condition. With advancements in medical interventions and rehabilitation programs, the outlook for patients with septal infarct continues to improve. By raising awareness about this condition and promoting a healthy lifestyle, we can contribute to reducing the burden of septal infarct and promoting heart health in the community.
Word Count: